Introduction: Despite some long-term remissions, eventual drug resistance in most patients remains a critical obstacle in the treatment of multiple myeloma (MM). The development of new drugs/drug combinations with novel mechanisms of action are needed for continued improvement in patient outcomes. Initiation of tumor cell death via activation of the intrinsic (mitochondrial) and/or extrinsic (death receptor) apoptotic signaling pathways has been shown to be an effective therapeutic strategy in MM. Venetoclax (Ven) is a selective, small-molecule inhibitor of BCL-2 that exhibits clinical activity in MM cells, particularly in patients harboring the t(11;14) translocation. Navitoclax (Nav) is a small-molecule that targets multiple antiapoptotic BCL-2 family proteins, including BCL-XL, BCL-2, and BCL-W to initiate the intrinsic apoptotic pathway. Eftozanermin alfa (Eftoza) is a novel, second generation TRAIL receptor agonist that induces cell death via death receptor pathways and is under investigation in multiple solid and heme malignancies. In addition, the pan-BET inhibitor mivebresib (Miv) and the BDII selective BET inhibitor ABBV-744 have shown synergistic activity with Ven in cell line models of multiple heme malignancies. Results reported here describe ex vivo drug sensitivities and functional genomic analyses of Ven, Nav, Eftoza, Miv, and ABBV-744 alone or in combination with standard-of-care agents, including bortezomib, carfilzomib, panobinostat, daratumumab, or pomalidomide.
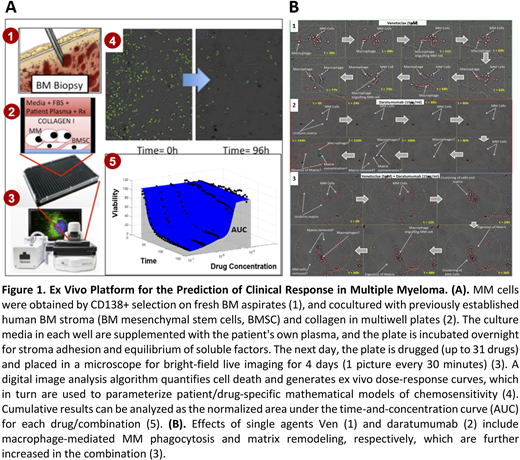
Methods: A high-throughput ex vivo drug screening assay using a coculture system of bone marrow (BM)-derived MM and stromal cells was used to assess the sensitivity of MM patient tumor cells (Figure 1A). Paired whole exome sequencing (WES) and RNA sequencing (RNA-seq) analyses were performed.
Results: Primary MM patient specimens (n=52) were evaluated in the ex vivo platform, including treatment-naïve, early relapse (1-3 prior lines), and late relapse (4-8 prior lines) patients treated with proteasome inhibitors, immunomodulatory drugs, and monoclonal antibodies. As expected, t(11;14)-positive MM patient specimens were more sensitive than wildtype to Ven ex vivo (D AUC, -18.6, P=0.002), however MM cells harboring amp(1q) were more resistant than wildtype (D AUC, +5.07, P=0.032), suggesting MCL1 (1q21 gene locus) is a key resistance factor to Ven single-agent activity in MM. Gene set enrichment analysis identified B-cell receptor signaling (normalized enrichment score (NES), 1.96, adjusted P=0.010) and MYC pathway (NES, 1.95, adjusted P=0.010) overexpression as predictors of increased sensitivity to Ven ex vivo. A t(11;14) gene expression signature was also generated using a penalized regression model approach in an additional MMWG/ORIEN MM patient cohort (n=155). The t(11;14) predictive gene expression signature was confirmed by correlation with Ven AUC in the ex vivo model. Additional pathway analyses were performed to identify potential predictive markers of sensitivity/resistance for each single agent and drug combination.
Although ex vivo activity of Nav was higher in t(11;14) specimens compared to non-t(11;14) (D AUC, -17.8, P=0.011), ex vivo activity in non-t(11;14) specimens was also observed, indicating additional anti-MM activity by cotargeting of BCL-XL and BCL-2. Both Miv and ABBV-744 showed single-agent activity ex vivo, however Miv demonstrated higher activity (median LD50=88.4nM), suggesting that pan-BET inhibition is more effective than BDII-specific BET inhibition in MM. Finally, a novel drug-combination effect analysis was used that identified novel synergistic ex vivo combinations including Ven and panobinostat (P=0.0013) and Eftoza with bortezomib (P=1.8E-7) or carfilzomib (P=7E-4). Additionally, single-agent induction of macrophage-mediated phagocytosis was observed in both Ven and daratumumab, which was synergistic when the 2 drugs were combined (Figure 1B).
Conclusion: An ex vivo functional genomic screen of MM patient specimens demonstrated the usefulness of this approach to identify candidate drugs and potential predictive biomarkers for continued evaluation in clinical trials. This approach confirmed known mechanisms of drug sensitivity and identified new ones, including a novel characterized immune-mediated synergy between Ven and daratumumab, and potential combination strategy for Eftoza and proteasome inhibitors.
Siqueira Silva:Karyopharm: Research Funding; NIH/NCI: Research Funding; AbbVie: Research Funding. Kulkarni:M2GEN: Current Employment. Mitchell:AbbVie: Other: payment for bioinformatics analysis, Research Funding; M2GEN: Current Employment, Research Funding. Dai:Cygnal Therapeutics: Current Employment; M2GEN: Ended employment in the past 24 months. Hampton:M2GEN: Current Employment. Lu:AbbVie: Current Employment, Current equity holder in publicly-traded company. Modi:AbbVie: Current Employment, Other: may own stock or stock options. Motwani:AbbVie: Current Employment, Current equity holder in publicly-traded company. Harb:AbbVie: Current Employment, Other: may hold stock or stock options. Ross:AbbVie: Current Employment, Current equity holder in publicly-traded company. Shain:Celgene: Honoraria, Membership on an entity's Board of Directors or advisory committees, Speakers Bureau; GlaxoSmithKline: Speakers Bureau; Sanofi/Genzyme: Honoraria, Membership on an entity's Board of Directors or advisory committees, Speakers Bureau; Karyopharm: Research Funding, Speakers Bureau; AbbVie: Research Funding; Takeda: Honoraria, Speakers Bureau; Janssen: Honoraria, Speakers Bureau; Amgen: Speakers Bureau; Adaptive: Consultancy, Honoraria; BMS: Honoraria, Membership on an entity's Board of Directors or advisory committees, Speakers Bureau.
While this is a preclinical study, venetoclax for treatment of multiple myeloma is not an approved indication
Author notes
Asterisk with author names denotes non-ASH members.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal